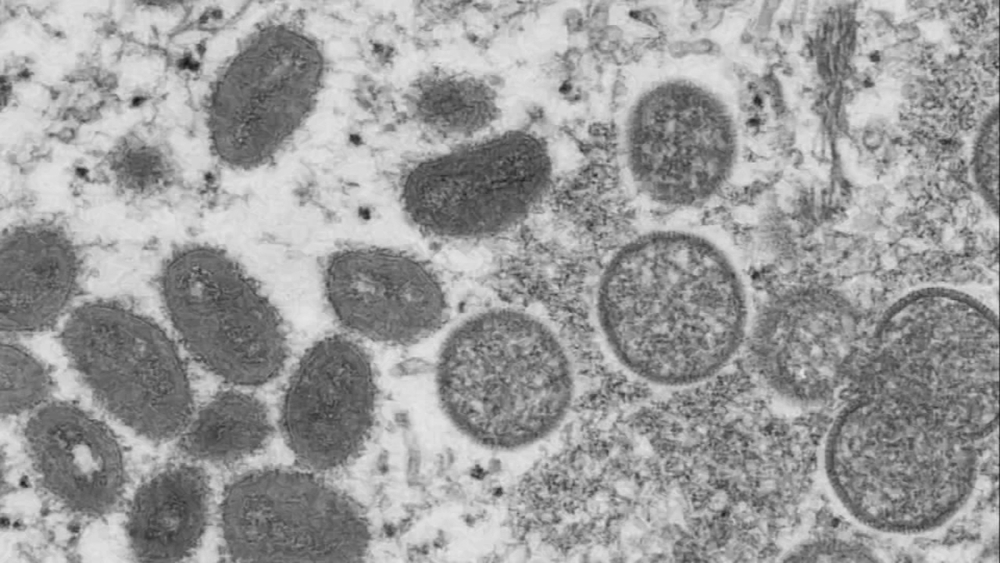
Monkeypox: Everything you need to know about origin, infection, vaccines, and treatment

SAN FRANCISCO (KGO) -- Monkeypox is currently spreading, and many people have questions. We've collected information from the Centers for Disease Control, the World Health Organization, and other trusted medical institutions to bring you some answers.
LIST: See open San Francisco monkeypox vaccine sites here
LIST: See open Alameda County monkeypox vaccine sites here
LIST: See open Contra Costa County vaccine sites here
LIST: See open Marin County monkeypox vaccine sites here
LIST: See open Napa County monkeypox vaccine sites here
LIST: See open San Mateo County monkeypox vaccine sites here
LIST: See open Santa Clara County monkeypox vaccine sites here
LIST: See open Santa Cruz County monkeypox vaccine sites here
LIST: See open Solano County monkeypox vaccine sites here
LIST: See open Sonoma County monkeypox vaccine sites here
While many of the new cases have been reported between men who have sex with men, monkeypox is not a sexually transmitted infection (STI). Anyone who has skin-to-skin contact with an infected person is at risk of contracting monkeypox.
ABC has confirmed that at least two children have been infected with the virus. One is a toddler in California, and the other is a baby who does not live in the U.S.
What is monkeypox?
Monkeypox is a zoonotic disease, meaning it is spread from animals to humans. According to the World Health Organization, it has been identified in certain monkey species, tree squirrels, dormice and more, and has spread mostly in Central and West Africa. It is now spreading in Europe and the United States.
Where did monkeypox come from?
In 1970, the first human monkeypox case was recorded in the Democratic Republic of the Congo in Africa, the WHO said in a fact sheet. Cases had been reported only on the continent until 2003 when one was recorded in the U.S., according to the agency. This outbreak resulted in more than 70 cases nationwide at the time.
The World Health Organization tells the Associated Press that the current outbreak is believed to originate from sex that happened at raves in Europe.
VIDEO: Man recovering from monkeypox describes symptoms, experience; doctor answers questions

Is monkeypox deadly?
Most people recover from monkeypox on their own within a month. However, the infection can be more severe -- some deaths have been reported in West Africa from the disease. Those with underlying health conditions may be at a greater risk for severe disease or death. Health authorities in the United Kingdom, where some of first cases were discovered in this recent outbreak, report that overall, the risk of death to the general population remains very low.
That said, monkeypox can lead to other medical problems, some of which can be deadly -- including pneumonia and infections in your brain and eyes.
How does monkeypox spread?
Generally, monkeypox spreads after direct contact with bodily fluids or skin lesions from an infected animal or person, according to the WHO. The CDC reports it can also spread from person to person through:
- Contact with infected rashes and scabs
- Respiratory secretions, including during close physical contact or touch such as kissing
- Touching areas that have come into contact with an infected person's rashes or fluids
- Additionally, an infected pregnant person can spread monkeypox to the fetus, according to the CDC
The California Department of Public health warns that monkeypox can also be spread by:
- Contact with contaminated materials (towels, bedding and clothing)
- Respiratory droplets spread by close and prolonged face-to-face interaction
Monkeypox is much less contagious than COVID-19.
VIDEO: How SF's responding to influx in monkeypox cases as demand increases for vaccines

Is monkeypox a sexually-transmitted infection?
Technically no, but it can be transmitted during sex because it spreads through close, intimate contact. The CDC says it is unclear if monkeypox can be spread through semen or vaginal fluids. You do not need to have sex to spread monkeypox. Skin to skin contact when one person is actively contagious is the main way that monkeypox spreads. Monkeypox CAN spread from linens / sheets / surfaces or through droplets when people are close for prolonged time. But specialists tell us these secondary modes of transmission are very uncommon.
Monkeypox spreads through close skin-to-skin contact, which means anyone can get it through physical contact. In the case of children, the CDC says could include holding, cuddling, feeding, as well as through shared items such as towels, bedding, cups, and utensils.
Who can get monkeypox?
Anyone who has been exposed to monkeypox can be infected. Symptoms usually show up within two weeks of skin-to-skin contact.
Many of the images of monkeypox shown on TV are of Black people. Are Black people more likely to get the virus?
No. The current outbreak outside of Africa has been mostly among white men who have sex with men. Because the virus is rare outside of Western and Central Africa, we have few images of the virus.
Because the cases have historically been on the African continent, and the majority of the population where outbreaks have happened is Black, most of our modern imagery shows people with darker complexions. ABC7 News has been working to collect images that are more reflective of the current outbreak's demographics.
What are the symptoms of monkeypox?
Symptoms of a monkeypox infection usually start out as flu-like and include chills, body aches and a fever. After a few days, a rash will appear, most often on the hands, face or pelvic region, according to the CDC.
The most common symptoms include:
- Rash
- Fever
- Headache
- Muscle aches
- Swollen lymph nodes
- Chills, fatigue
According to the CDC, monkeypox rashes appear differently throughout its stages and can look like pimples or blisters, and not necessarily in the location where the initial contact was made. The resulting rash may be found on the face, mouth or anywhere else on the body. Patients report that the sores are excruciatingly painful and often itchy.
What should you do if you have monkeypox?
The California Department of Health of makes the following suggestions if you have monkeypox:
- Always stay home if you're sick
- Cover any blisters or skin lesions
- Isolate from others and wear a mask if you have to be around others
- Contact a health care provider right away to talk about diagnosis, testing, and treatment options
Is there a vaccine?
Yes. There are two vaccines available. Jynneos is specifically made to prevent monkeypox. It is delivered by a shot to the arm. Two doses are needed to complete the vaccination.
The smallpox vaccine ACAM2000 can also be used to prevent monkeypox, but it cannot be used on people with certain medical conditions and has known side effects. It is given with a two-pronged needle. The resulting scratch turns into a blister. Because the vaccine contains live smallpox virus, it can be spread to other parts of the body, or other people.
"We have 100 million doses of ACAM2000," National Institute of Allergy and Infectious Diseases Director Dr. Anthony Fauci said in late June, but its side effects mean that it "in my mind, as a public health person, would not be worth giving it widely throughout the general population."
How is monkeypox diagnosed?
Because monkeypox is rare, there are no tests to determine if you have the disease until the open sores appear. To diagnose a monkeypox infection, a healthcare provider will take a tissue sample from an open sore and send it to a lab for genetic testing or a PCR test. This is the same process used to determine if you have a COVID-19 infection. You may also need to give blood to check for antibodies in your system.
How is monkeypox cured? Can it be treated?
You should consult your doctor or visit urgent care if you believe you have monkeypox. There are no approved antiviral drugs to treat monkeypox, and there is limited research on whether existing antiviral drugs will help patients recover. Most people with monkeypox will recover on their own within four weeks. Most patients report permanent scarring.
Should I go to the ER or urgent care?
If you feel you need urgent medical attention, contact your doctor. According to the Cleveland Clinic, some symptoms that may warrant a trip to the ER are:
- Trouble breathing
- New or worsening chest pain
- Stiff neck
- You are confused or can't think clearly
- Difficulty speaking or moving
- Loss of consciousness
- Seizures
Do you need the monkeypox vaccine?
The CDC currently is recommending that people exposed to monkeypox or people who are at high risk for contracting the disease should get the vaccine. The vaccine is delivered in two doses, four weeks apart. People who have already received the smallpox vaccine may only need one shot.
Booster doses are recommended every two or 10 years if a person remains at continued risk for exposure to smallpox, monkeypox, or other orthopoxviruses. Your health care provider can give you more information.
The CDC reports "Smallpox was declared eradicated in 1980 and no cases of naturally occurring smallpox have happened since 1977."
The CDC said you may want to consider getting the monkeypox vaccine if:
- You were in close contact with an infected person
- You engaged in sexual activities with someone who was diagnosed with monkeypox in the past two weeks
- You have had multiple sexual partners in an area where monkeypox is spreading
Where can you get the monkeypox vaccine?
San Francisco officials released a list of open monkeypox vaccine sites here.
Who should get the monkeypox vaccine?
If you know you have been exposed to monkeypox, the CDC advises getting your first shot within four days of exposure.
The World Health Organization announced in a news released on May 25, 2022 that the current outbreak has been identified within gay and bisexual communities and among men who have sex with men. However, "it is important to note that the risk of monkeypox is not limited to men who have sex with men," the agency said.
San Franciscans who are eligible for a Jynneosvaccine are:
- Gay, bisexual, and other men who have sex with men and trans people who have sex with men and have had multiple (more than one) sexual partners in past 14 days
- Sex workers of any sexual orientation/gender
- Identified as a close contact of someone who has monkeypox (suspected or confirmed)
- Received a notification from a venue or event of a potential exposure to someone who has monkeypox (suspected or confirmed)
- A laboratory worker who routinely handles monkeypox virus samples for diagnosis or testing purposes or any clinician who has a high-risk occupational exposure
Who should not get the vaccine?
The vaccine should be avoided by those with cardiac disease, eye disease being treated with topical steroids, weaker immune systems, skin conditions such as eczema or those who are pregnant, the agency said.
What is the monkeypox vaccine?
Smallpox/monkeypox vaccine (JYNNEOS) can prevent smallpox, monkeypox, vaccinia, and other diseases caused by orthopoxviruses. JYNNEOS is approved by the Food and Drug Administration (FDA) for prevention of smallpox and monkeypox disease in adults 18 years or older at high risk for smallpox or monkeypox infection. The vaccine is made using weakened live vaccinia virus and cannot cause smallpox, monkeypox, or any other disease.
What does monkeypox have to do with smallpox?
The most widely used vaccine approved to prevent monkeypox is also used to prevent smallpox. Doctors declared smallpox extinct in the United States in 1952, in large part because of widespread vaccination. At the height of the epidemic three in 10 people died from the virus, many others were disfigured, according to the CDC. People who have been vaccinated for smallpox are less likely to experience side effects of a new vaccination, and may only need one dose.
How do I know if I have already been vaccinated for smallpox?
In 1972, the smallpox vaccine was lifted from a list of routine vaccinations in the United States. One way you may be able to determine if you have had a smallpox vaccine is to look for a mark or scar on your upper arm. The distinctive scar left by the vaccine left a circular indentation in some people, smooth scars on others. The blemish is usually no bigger than a pencil eraser, though some people have large scars.
However, the smallpox vaccine wasn't the only vaccine to cause a scar. The Bacillus Calmette-Guérin, or BCG vaccine, protected people against human tuberculosis.
- If you were born after 1972, and have a scar, you likely got the BCG vaccine and not the smallpox vaccine
- If you were born in the United States, you likely got the smallpox vaccine
- If you were born in a country that had higher rates of TB, you likely got the BCG vaccine
- The BCG vaccine tends to be raised and rounded, the smallpox vaccine is usually a depression in the skin, has jagged edges, and is slightly rounded
How do I keep myself safe?
The CDC recommends avoid close contact or sharing personal objects with anyone who has monkeypox. If you have been near someone who has the disease, you are encouraged to wash your hands frequently.
The CDC says to avoid skin-to-skin contact in places where the virus may be present. That includes wearing long-sleeve shirts and pants to prevent contact with another person's skin. They also encourage people to avoid intimate contact, including sex, with anyone who has confirmed or suspected monkeypox. Condoms may prevent spread as well. o Having multiple or anonymous sex partners may increase your chances of exposure to monkeypox. Limiting your number of sex partners may reduce the possibility of exposure.
How can a person lower the chance of getting monkeypox at places like raves, parties, clubs, and festivals?
When thinking about what to do, seek out information from trusted sources like the local health department. Second, consider how much close, personal, skin-to-skin contact is likely to occur at the event you plan to attend. If you feel sick or have a rash, do not attend any gathering,
and see a healthcare provider.