Stanford doctors protest, voice concerns about their place in receiving COVID-19 vaccine

PALO ALTO, Calif. (KGO) -- More than a hundred Stanford Health Care resident physicians and fellows demonstrated against the rollout of their administration's COVID-19 vaccine plan Friday morning and voiced concerns about their place in the pecking order.
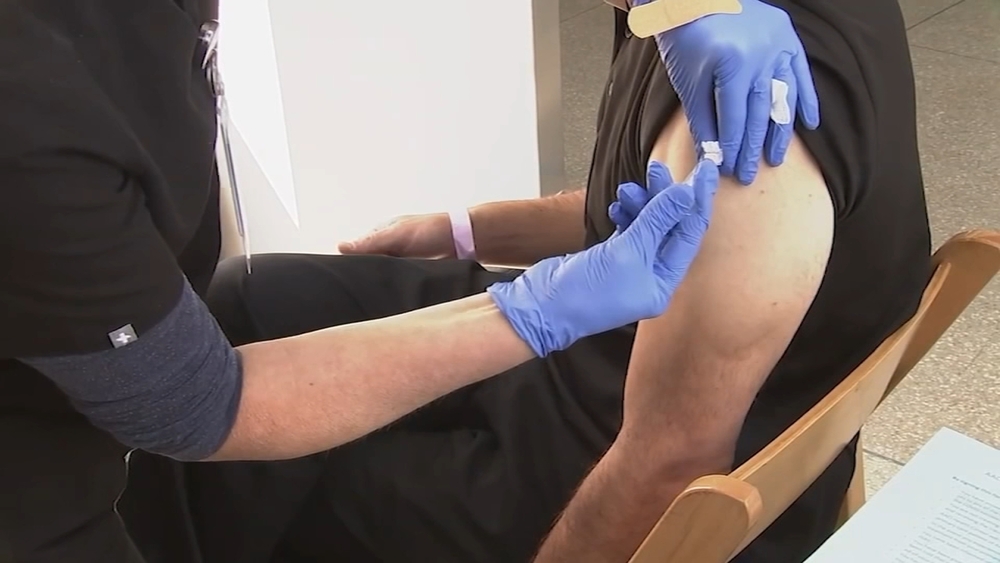
Residents are doctors in training who often work upwards of 80 hours per week and are often the first in line to treat patients with COVID-19, including in the emergency, as well as the ICU. But ahead of the hospital's plan to begin vaccinating its workforce this week, many were surprised to learn that they wouldn't be in the first wave.
RELATED: FDA grants emergency use authorization for Moderna's COVID vaccine
"To not be offered a vaccine when I am at the hospital, FaceTiming in attendings (physicians) from home so they can see their patients, and I am in the COVID-positive room, and those attendings are offered a vaccine, it's very hurtful," said Stanford resident physician Dr. Sarah Johnson.
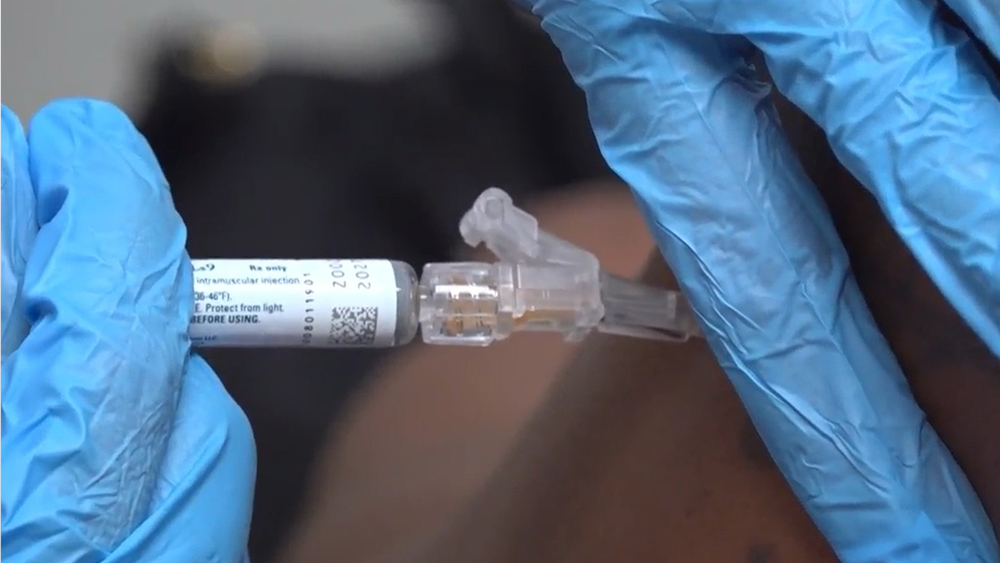
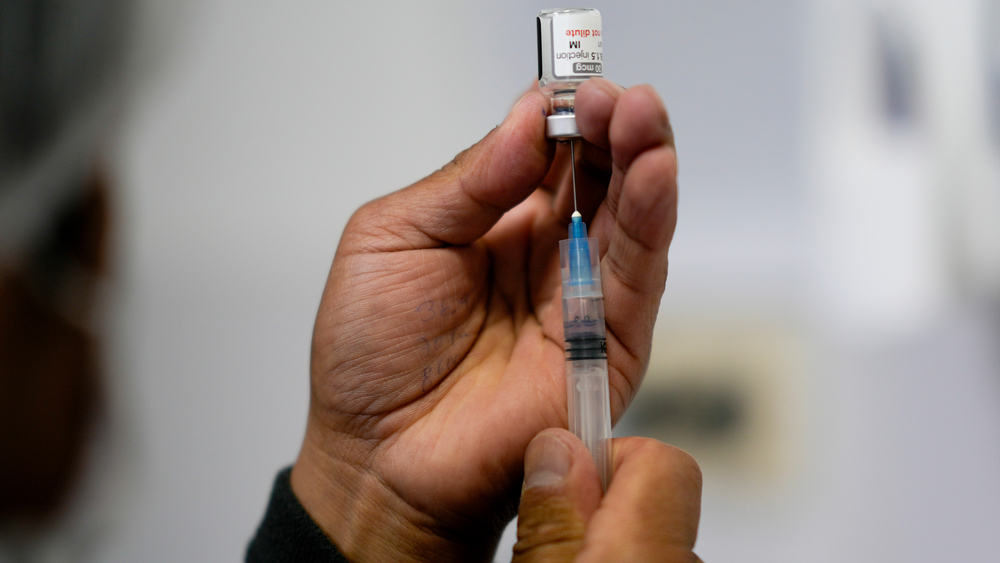
Stanford has received at least 3,900 doses of the Pfizer vaccine, but demonstrators say only seven out of 1,349 residents and fellows were given the chance to be vaccinated in the first round. They understand that supply is limited, but say their frustration stems from being told that priority was given to some faculty who are working from home and have no in-person patient responsibilities.
In a statement late Friday afternoon, Stanford Health Care said:
RELATED: COVID-19 vaccine has been distributed, what now?
"We take complete responsibility for the errors in the execution of our vaccine distribution plan. Our intent was to develop an ethical and equitable process for distribution of the vaccine. We apologize to our entire community, including our residents, fellows, and other frontline care providers, who have performed heroically during our pandemic response. We are immediately revising our plan to better sequence the distribution of the vaccine."
Resident physicians wanted to make clear that they're proud to be doing their training at Stanford, but felt that they had no other choice but to speak up. As trainees, they hope to have a seat at the table during future discussions surrounding patient care and workplace safety.
The Stanford protest underscores the broader issue of equity and ethics in the rollout of the vaccine and shines a light on the power that hospital administrators have in the decision making.
The CDC has determined access will be granted via a phased process while the vaccine supply is limited.
Currently, we are in Phase 1a. In California, the Department of Public Health (CDPH) has given guidance on sub-prioritization within that phase.
The first tier includes "Persons at risk of exposure to SARS-CoV-2 through their work in any role in direct health care or long-term care settings" according to CDPH. That includes employees in non-clinical roles such as environmental services, patient transport, or interpretation.
Once a facility has given access to those populations, they can move to tier 2, which includes primary care clinics, intermediate care facilities, home health workers and public health field staff.
But the Stanford rollout has showed once a health care system gets their allocation of vaccines, administrators get to decide how to weight their internal decisions.
"There isn't necessarily a right way of doing it. There are a lot of important factors," said Dr. Louise Aronson, a professor at UCSF and a member of the California Drafting Guidelines Workgroup, which helped advise CDPH on the tiered system.
She said some systems have created online questionnaires for employees to fill out, which have information that is weighted in an algorithm. Other facilities have created ranks purely based on other factors such as the age of employees or the site of their job.
She said even at the national level there are disagreements, especially for the next phase.
The National Academy of Medicine believes that all older Americans with comorbidities should be in the next phase, while the CDC's Advisory Committee on Immunization Practices believes essential workers should be prioritized after health care workers.
"You can see how two really educated groups can make very different decisions," said Aronson.
In the wake of the Stanford protest, Ali Bay, a spokesperson for CDPH, told ABC7 "The federal and state vaccine guidelines have prioritized our front-line health care workers who have been putting their lives at risk to fight this virus from day one. We urge all health care providers to follow the state's guidelines on vaccination phases which were created in consultation with experts and community leaders."
Get the latest news, information and videos about the novel coronavirus pandemic here
RELATED STORIES & VIDEOS:
- Map: CA counties that can, can't reopen under new rules
- VIDEO: When will I get the COVID-19 vaccine? We explain who goes 1st
- COVID-19 risk calculator: The safest and most dangerous things to do this holiday season
- Want to get a COVID-19 test in time for the holidays? Here's what you need to know
- Updated number of COVID-19 deaths, cases in Bay Area
- Map shows everywhere you can get a COVID-19 test in the Bay Area
- COVID-19 Diaries: Personal stories of Bay Area residents during pandemic
- California EDD: The most commonly asked questions we get about unemployment and PUA
- Health experts urge flu shots in effort to avoid 'twindemic'
- How to tell the difference between seasonal allergies and coronavirus symptoms
- Here's which mask is better to protect from COVID-19
- First COVID-19 vaccine volunteers in US describe experience as Bay Area launches vaccine trials
- Coronavirus origin: Where did COVID-19 come from?
- What is a COVID-19 genetic, antigen and antibody test?
- What will it take to get a COVID-19 vaccine and how will it be made?
- What does COVID-19 do to your body and why does it spread so easily?
- Here's how shelter in place, stay at home orders can slow spread of COVID-19
- Coronavirus Timeline: Tracking major moments of COVID-19 pandemic in San Francisco Bay Area
- Coronavirus Doctor's Note: Dr. Alok Patel gives his insight into COVID-19 pandemic